Tooth extraction, healing implantation (part 2)
Delayed implantation
In the last issue, we discussed four types of dental implant placement depending on the degree of soft tissue and bone healing, see the table below.
| Classification | Description | Period after tooth extraction | Clinical situation during implant placement |
| Type 1 | Immediate implantation | Immediately after tooth extraction | No healing of bone and soft tissue |
| Type 2 | Early implantation after soft tissue healing | About 4-8 weeks | Gingival healing but no bone healing |
| Type 3 | Early implantation after incomplete bone healing | About 12-16 weeks | Gingival healing and substantial bone healing |
| Type 4 | Delayed implantation | About 6 months or later | Complete tissue healing in the well area |
And mentioned that for a long time the gold standard was the fourth type – delayed implantation. Indeed – it is the easiest way to place an implant. In addition, almost the entire block of data on osseointegration, primary and secondary stability is derived from surgeries performed exactly according to the fourth type.
It is also the most reliable and affordable way to perform implants, which is recommended for all beginning dentists. Minimal stress for the dentist and therefore also for the patient.
There are clinical cases where no other type of implantation is allowed. Here are a few examples when it is imperative to give the body time, patch everything up, and restore the alveolar bone.
- When the indication for extraction was cystic masses or any other inflammatory processes affecting the bone tissue. In these cases, the tooth extraction is accompanied by the formation of huge cavities, and the implant simply has nowhere to be placed.
- When it is necessary to remove the molars of the upper jaw, the roots of the teeth protrude into the sinus. If even before removal it is clear that the height of the bone is small and most likely you will have to make a sine elevator, then it makes sense to wait. Time is needed for the body to level the tubercles and depressions at the bottom of the sinus. These irregularities were caused by the penetration of the roots of the teeth. If you do a sinus lifting operation right away, you need an extreme level of surgeon skill and a fair share of luck.
 It is much better to wait until the bottom of the maxillary sinus is completely aligned. Then you can safely peel off the Schneider’s membrane and insert the bone material.
It is much better to wait until the bottom of the maxillary sinus is completely aligned. Then you can safely peel off the Schneider’s membrane and insert the bone material. - When you want to do everything calmly and reliably with minimal risk of complications.
Nuances of tooth extraction and healing processes
The success of further implantation depends on how the tooth is extracted and what measures are taken to preserve the bone mass of the alveolar ridge. Let’s take it one step at a time.
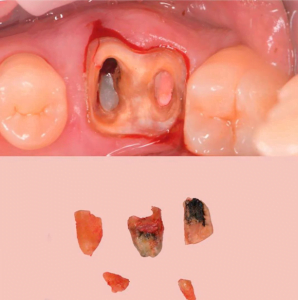
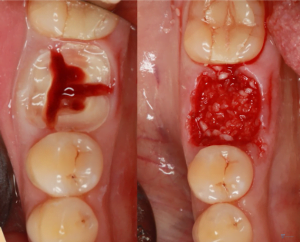
- Tooth extraction should be as minimally traumatic as possible in order to preserve the alveolar cavity as much as possible. This means that multirooted teeth must be sawed, see pictures below.
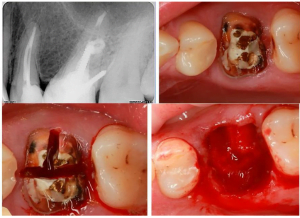 You need to turn a multi-rooted tooth into several single-rooted teeth and remove them one by one, which is undoubtedly much easier and safer. The alveolar wall is preserved as much as possible.
You need to turn a multi-rooted tooth into several single-rooted teeth and remove them one by one, which is undoubtedly much easier and safer. The alveolar wall is preserved as much as possible. - Although the tooth extraction was done correctly, several healing and alveolar ridge formation scenarios are possible. The first of the two images below shows a good option for subsequent implantation. Here you can see a good gingival profile, no dip on the vestibular side of the alveolar ridge and therefore no augmentation is required.
The situation is quite different in the lower image. After healing, there is a sag on the vestibular side (the concave part of the gingiva, indicated by the blue curved line). All practicing dentists must have seen this gap and know that resorption of the alveolar ridge is always more pronounced on the external (vestibular) side.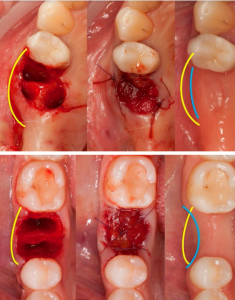 One or the other type of healing is significantly influenced by the congenital phenotype. Namely: thick, thin or medium, which can be easily distinguished by the width and massiveness of the attached keratinized gingiva. The biological phenotype affects not only the height of the papillae and the massiveness of the gingiva, but also the thickness of the alveolar portion and the overall massiveness of the bone.
One or the other type of healing is significantly influenced by the congenital phenotype. Namely: thick, thin or medium, which can be easily distinguished by the width and massiveness of the attached keratinized gingiva. The biological phenotype affects not only the height of the papillae and the massiveness of the gingiva, but also the thickness of the alveolar portion and the overall massiveness of the bone.
Those with a thick phenotype have a bone deficit for root implants much less frequently. What to do if the bone deficit is still significant is discussed below.
What spatial changes the alveolar crest undergoes after the tooth is removed
We need to understand what happens to the alveolar bone during the healing process to predict whether horizontal augmentation will be necessary. We discussed the basics of the healing process in the first part of our review.
Now let’s figure out what is happening with the volumes in the oral and vestibular parts of the alveolar bone. To do this, let’s turn to the study of doctors Araujo and Linde from 2005.
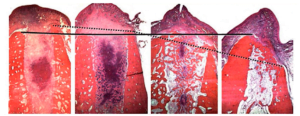
The histological section below clearly shows that the height of the alveolar wall is almost unchanged on the oral side, see the solid line in the illustration below. Whereas the vestibular wall is dissolved to a large extent, see the dotted line.
This results in a relatively sharp ridge and a noticeable horizontal bone deficit. If you try to insert an implant into such a bone, several coils on the vestibular side will not be covered by bone. Horizontal augmentation (bone augmentation) is indicated for such clinical cases.
How to Change the Comb Remodeling Scenario
Observations of the aforementioned phenomenon of loss of ridge width have led to an increase in the popularity of the second type of implantation. Indeed, it makes sense to place an implant before a significant amount of bone is lost and preserve it in this way. But today we will look at the essence and effectiveness of techniques to reduce bone loss.
All the techniques that dentists use to intervene in the healing process and preserve bone mass have their origins in ridge reconstruction techniques.
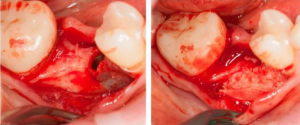
For example, the image below shows a noticeable loss of bone mass from the side of the cheek. And the adjacent picture shows the process of horizontal augmentation, namely the bone material (graft) with a fixing membrane.
This is a well-established and quite effective procedure that allows you to obtain even excess bone. The picture below shows bone growth even outside the bone envelope.
A logical question arises. If you build up bone tissue when the tooth has been gone for a long time, then why not do something similar immediately after removing the tooth.
After all, every surgical intervention is a risk, not to mention a loss of time. First, it takes several months for the bone to heal, then it will be found that the width of the alveolar crest is insufficient, and a decision is made on augmentation. After that, several more months pass before implantation.
To avoid such a long course of treatment, procedures appeared aimed at preserving the well and preserving the width of the alveolar crest after healing. Let’s figure out in more detail what can be done immediately after the tooth is removed to preserve the alveolar crest.
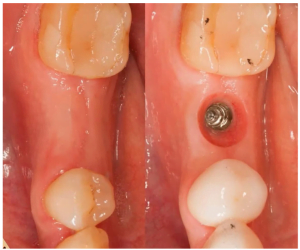
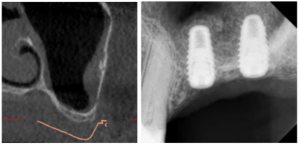
Before proceeding to the results of the studies, let’s analyze one case, see the photo below. The case is taken from open sources. We see a competently removed molar of the upper jaw.
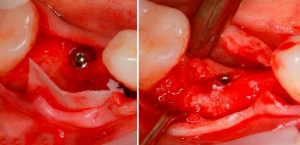
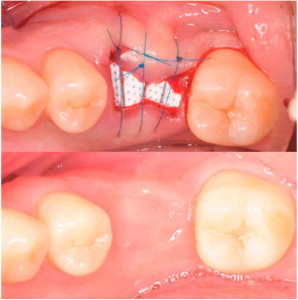
You can see from the scans that the doctor did a competent fragmentation and removed the roots of the tooth. And immediately after the extraction, an alveolar ridge augmentation surgery was performed, see pictures below.
Unfortunately, we do not know what bone material was used, but we can see that PTFE membrane (non-resorbable barrier membrane) was used. As you can see the surgery was successful the healing of bone and soft tissue was perfect for implantation.
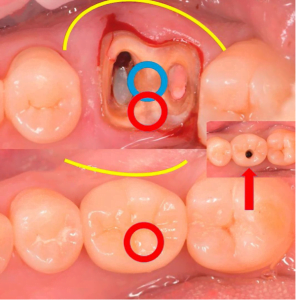
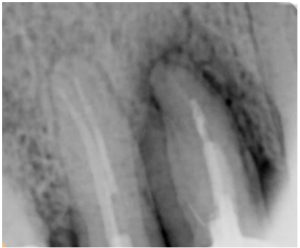
But then for some reason, the doctor placed the implant with a significant displacement to the oral wall. The healed area showed that the implant could have been placed in the center. The pictures below show the red circle showing the actual location of the crown to abutment and the blue circle shows the recommended location.
This raises the question of why the dentist did this. Everything shows an experienced hand. Perhaps the operation to save the ridge was not as successful as it seems at first glance, perhaps there was another reason.
Let’s try to figure out how much the procedure for preserving the alveolar ridge “unties the hands” of the dentist. To do this, we turn to research. Although it is quite difficult to understand this issue. There is a lot of conflicting data, and the statistical material for the meta-study was collected only by 2014. The very methods of preserving the alveolar ridge began to be used at the beginning of the 2000s.
We will first look at a systematic review from 2014.
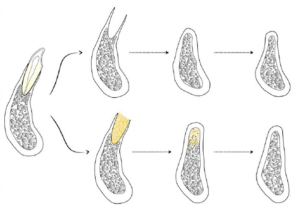
The illustration below shows the difference between alveolar ridge formation: the upper row is when the tooth was extracted and nothing was done. The lower row is when bone material was placed in the hole.
The results show that in the second case, the height and width of the alveolar ridge were largely preserved. This study unequivocally states that alveolar ridge preservation techniques work. Specifically, alveolar bone loss occurs either way. But in the case of preservation procedures, the average loss of alveolar ridge width is – 1.83 mm less.
This is quite a lot, because if the width of the alveolar ridge is 6 mm in the molar region, then it is no longer possible to place an implant with a diameter of 4 mm. And if it were possible to maintain a width of 6 + 1.83 = 7.83 mm, then this is already a good indicator and a 4-mm implant can be confidently placed.
But even here it was not without pitfalls. Here are the main conclusions that can be drawn from this study.
- Alveolar ridge preservation procedures give a positive result.
- the study was conducted only on the area from premolar to premolar. The study did not include the masticatory teeth.
- it could not be determined precisely which bone material worked better. It was noted, however, that xenografts and allografts worked be
- tter.
Despite the effectiveness of the techniques, there is always the possibility of failure. And in some cases you still have to do additional augmentation after healing. And this is important for the patient, the dentist, and the insurance company employee to know. If it turns out that bone grafting is needed anyway, it’s not because the doctor did something wrong. And this procedure is paid for separately.
What is better for preserving the well: xenografts, allografts or PRF
We have already seen the general effectiveness of alveolar ridge preservation techniques. Now we need to find out exactly how effective they are and which materials show the best results.
As we have already mentioned, it works best:
- xenografts – material of animal origin – bovine, equine, porcine especially parts with low resorption modulus;
- allografts – material of cadaveric origin, in particular the use of the cortical part of the donor bone.
Alloplastic materials work much worse – completely artificial ones based on calcium triphosphate and hydroxyapatite.
All of the above materials are also used in classical augmentation procedures. From this we can make a generalizing conclusion that the procedures for preserving the alveolar ridge are a special case of augmentation.
Now let’s move on to the main and most recent study on this topic.
This is a fresh meta-analysis of the Cochrane group, which Dr. Atieh did with colleagues in 2021. It’s all about interventions after teeth are removed. That is, preparing the alveolar crest to preserve the maximum bone tissue and prepare for implantation.
This study is valuable in that both pre-existing previously systematic analyses and statistics on new clinical cases were used for it.
Here are the conclusions, and they are discouraging:
- Alveolar ridge preservation techniques can minimize overall changes in residual ridge height and width six months after extraction, but the evidence is very inconclusive.
- There is no evidence of any difference:
– in the need for additional augmentation during implant placement;
– failures, aesthetic outcomes, or any other clinical parameters due to lack of information or long-term data.This means that it is not possible to track the percentage of cases where additional augmentation will have to be performed after preservation measures. - There is no evidence of any clinical difference between the different materials and membranes used for alveolar ridge preservation. Although data can be found within the study that xeno and allo materials produce the best results. More precisely, they cause the least number of complications.
To be honest, the results are not what I would like to get, but the wording could not be clarified because insufficient data is not a verdict. Surely new studies and new methods will appear in the near future, which will show unambiguous results.
Before we get to the final conclusions, let’s look at one more material and technique. Namely, platelet-rich plasma.
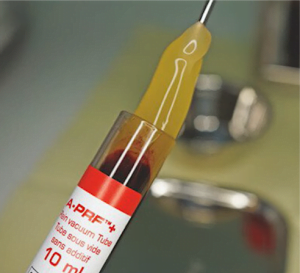
At the beginning of the spread of this technique there were enthusiastic sentiments that platelet-enriched plasma PRF could replace the membrane and almost the bone graft itself. Sellers of centrifuges and related products were especially fond of telling about it.
In fact, it turned out that platelet-rich plasma has no effect on bone healing. Neither harm nor benefit.
Still, the use of PRF plasma is not the pure child of marketing. It is successfully used to protect the blood clot immediately after extraction. And it practically reduces the risk of alveolitis to zero.
And that’s a lot, because alveolitis causes not just discomfort, but severe pain. And the treatment of alveolitis is quite complex and time-consuming.
Is it possible to save bone after removal
Let’s try to summarize. And find out why it is so difficult with certainty, because at the beginning of 2022 there were no clear correlations. To begin with, let’s formulate what we know for sure.
- There is no harm or danger in alveolar ridge preservation procedures. And they either help preserve the ridge or you have to do additional augmentation anyway.
- Many individual studies and the statistics they have collected have been categorized as low confidence data. This is because most of the studies showing positive results were funded by the membrane and bone material companies. Therefore, the validity of the data has been questioned. This does not mean that they are wrong and there are no positive results, just that they did not play a sufficient role in the statistics. The goal of the scientific approach is objectivity.
- Each specialist can rely on his own experience of practice and the results of research in the quality of which he does not doubt.
We have a rather positive attitude toward bone ridge preservation techniques. As confirmation, here is another qualitatively done study where there were test and control groups and a blind distribution.
The only comment on the quality of the results was that the difference in bone loss on the lingual and vestibular sides was not shown. This is important for subsequent implantation.
The alveolar ridge preservation procedure was performed according to the standard procedure using OsteoBiol bone graft and membrane.
| Horizontal bone loss | Vertical bone loss | The need for bone augmentation | |
| Control group | 3,6 ± 0,72 mm | 2,1 ± 0,6 mm | 42% |
| Test group | 1,6 ± 0,55 mm | 1,1 ± 0,96 mm | 7% |
As we can see, the probability of augmentation in the test group is only 7%, whereas if nothing is done, after six months almost half of the patients will have to undergo augmentation.
At first glance, everything looks great, except for the financial issue. After all, an elementary extraction is relatively inexpensive. And a tooth extraction with an alveolar ridge preservation procedure is 2-3 times more expensive.
If you look at the statistics from the other side, it turns out that the majority of patients did not need the preservation procedure.
For example, there are two groups of 100 patients each. It turns out that the control group underwent the bone augmentation procedure only in 42 cases, the remaining 58 patients did not need the primary or additional procedures.
And in the test group, intervention was performed 107 times – (7 cases twice). From a financial point of view, the group of patients where the alveolar ridge preservation procedure was performed would bring in more than 2.5 times more money compared to the control group. Or if you evaluate on the other hand the patients will spend several times more.
Therefore, the final conclusions and recommendations from us will be.
- The preservation procedure is safe and moderately effective. To do or not to do it should be decided each time individually. There are patients who are ready to pay more to reduce the risk of additional surgery, and there are people who are ready to take a risk, because the probability that augmentation will not be necessary, even if nothing is done, is over 50%.
- It’s imperative to inform the patient about all the benefits and risks. Especially the likelihood that bone augmentation surgery may still be necessary. The additional augmentation will be paid for by the patient or the insurance company, since the need for repeated intervention is not a guarantee.We hope you found this article helpful. Until future publications.
-
Zimmer Biomet® Compatible Screw Retained Restoration Trial Kit + Dental Implant
Original price was: $134.$9.90Current price is: $9.90. Buy Now -
Zimmer Biomet® Compatible Screw Retained Restoration Trial Kit
Original price was: $70.$0.99Current price is: $0.99. Buy Now -
Zimmer Biomet® Compatible Cemented Restoration Trial Kit + Dental Implant
Original price was: $114.$9.90Current price is: $9.90. Buy Now -
Zimmer Biomet® Compatible Cemented Restoration Trial Kit
Original price was: $50.$0.99Current price is: $0.99. Buy Now