Linking menopause and dental health: what dentists need to know
Menopause is a period in a woman’s life when there are hormonal changes associated with the decline of reproductive function. Menopause can be accompanied by many unpleasant symptoms, including affecting the condition of the teeth and soft tissues of the mouth. We will not cover here methods of managing menopause symptoms, such as hormone replacement therapy. Each woman can consult with an endocrinologist on these issues. Here we will also consider what recommendations and procedures dentists can offer to reduce the risk of problems with teeth and gums.
Dry mouth
Decreased estrogen levels during menopause can cause a decrease in saliva production. Lack of saliva can lead to dry mouth (xerostomia), which increases the risk of tooth decay, gum inflammation, and other dental problems. Dry mouth can also reduce quality of life by causing discomfort, making it difficult to speak, swallow, and decreasing taste sensation.
What to do
Advise menopausal women to drink enough water, use oral moisturizers, avoid alcohol, caffeine, tobacco, and spicy foods, and perform regular dental and gum hygiene.
Gum changes
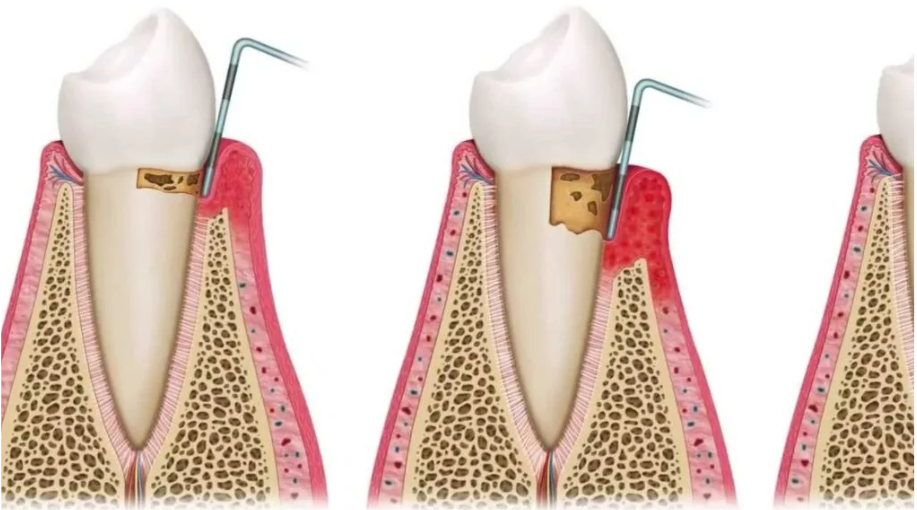
Hormone levels can affect gum health. Menopausal women have an increased risk of developing gingivitis (inflammation of the gums) and periodontitis (inflammation of the tissues surrounding the teeth) due to decreased blood supply to the gums. Changes to the gums can manifest as redness, swelling, bleeding, pain, deepening of the spaces between the teeth, and tooth mobility.
What to do
Have regular checkups and professional cleanings of the teeth and gums, prescribe antibacterial and anti-inflammatory medications, and bite-correcting procedures. It is also important to follow a proper diet rich in calcium and vitamin D, which help strengthen bone tissue. But be careful prescribing high doses of vitamin D can lead to calcium deposition in the blood vessels, so also prescribe vitamin K complex and other related supplements that will help calcium and vitamin D to be absorbed properly.
Osteoporosis
Changes in bone density also increase the risk of periodontal disease. Osteoporosis is a condition in which bones become more brittle and prone to fractures. Osteoporosis can affect not only the spine, hips and wrists, but also the jaws. It can lead to tooth loss, reduced effectiveness of implants, and changes in facial shape.
What to do
Dentists can diagnose osteoporosis through jaw x-rays, bone density measurements, and blood tests for calcium and phosphorus levels. Treatment for osteoporosis may include calcium, vitamin D and bisphosphonate medications, as well as exercise and avoidance of smoking and alcohol.
Appearance of ulcers
Hormone levels can also affect the oral mucosa, which can lead to ulcers and more sensitive mucosa. Ulcers can be caused by irritants such as dentures, toothbrushes, floss, hot or spicy foods, as well as stress, infections, or allergies. Ulcers can cause pain and discomfort, as well as make eating and oral hygiene difficult.
What to do
Dentists can treat ulcers with topical anesthetics, antiseptics, antifungal or antibiotic agents, and adjust dentures or orthodontic appliances as needed. It is also recommended to avoid traumatic factors, drink enough water, eat soft and neutral foods, and consult a doctor if there are any comorbidities.
Conclusion
Menopause is an important stage in a woman’s life that requires special attention to health. Dentists can help menopausal women maintain their dental and oral health, prevent and treat potential problems, and improve their quality of life. This requires regular dental visits, hygiene, nutrition and lifestyle habits, as well as consultation with a gynecologist and endocrinologist when necessary.