Dental implantation in systemic diseases: opportunities and limitations
Despite the effectiveness and sophistication of the technology, dental implantation is not available to all patients. Contraindications can be both temporary and permanent. Today, we will talk about what systemic diseases can affect the results and safety of implantation. For more detailed insights, consider this comprehensive article on risk factors and contraindications for dental implantation.
What systemic diseases lead to contraindications to dental implantation
Here are the most common systemic diseases that make dental implantation impossible or extremely risky for the patient:
- Cancer. Patients who have been diagnosed with cancer or are receiving chemotherapy or radiation therapy cannot have dental implants because it may worsen their condition, cause complications, or reduce the effectiveness of treatment. Dental implants may be considered only after the cancer has been completely cured or remission has stabilized.
- Immunodeficiency conditions. Patients with congenital or acquired immunodeficiencies, such as HIV infection, cannot have dental implants because they have an increased risk of developing infectious complications, implant rejection, or failure to osseointegrate.
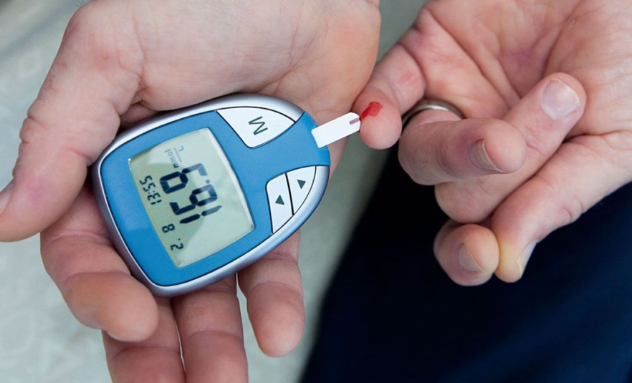
- Diabetes mellitus. Patients with unstabilized diabetes mellitus can not do dental implants because they have reduced regenerative capacity of tissues, metabolism and blood circulation, which can lead to delayed wound healing, infection of implants or their loss . Patients with compensated diabetes mellitus can have dental implants provided that blood glucose levels are strictly controlled and all medical recommendations are followed.
Systemic diseases that are limitations for dental implants
There are some systemic diseases that are not absolute contraindications for dental implants, but require a special approach and prior preparation. Such diseases include:
- Cardiovascular diseases. Patients with coronary heart disease, arterial hypertension, arrhythmias, heart defects or implanted pacemakers can have dental implants provided that their condition is well compensated, they consult with a cardiologist and prevent endocarditis.
- Osteoporosis. Patients with osteoporosis can undergo dental implantation provided that they have sufficient bone density, no history of fractures and discontinuation of bisphosphonates 3 months prior to surgery.
- Hematologic disorders. Patients with blood clotting disorders, anemia, leukemia or other blood diseases can undergo dental implantation provided that their blood parameters are corrected, they consult with a hematologist and prevent bleeding.
What we can offer for patients with systemic diseases
Patients with systemic diseases who cannot have dental implants or who have a high risk of complications should not despair and resign themselves to missing teeth. There are other options for restoring lost teeth, such as:
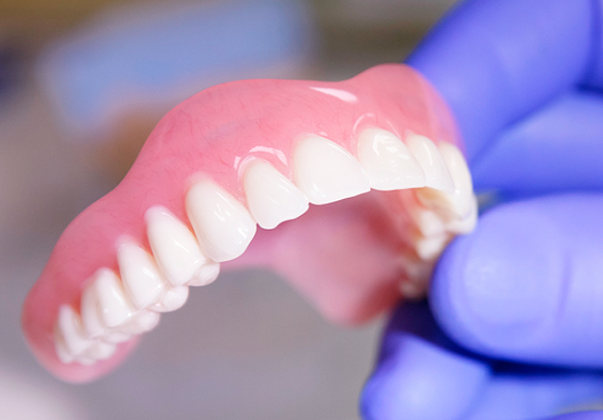
- Removable Dentures. Removable dentures are the easiest and most affordable way to replace missing teeth that does not require surgery and has no contraindications. Removable dentures can be partial or full, acrylic or nylon, removable or removable . Removable prostheses allow to restore the aesthetics and function of teeth, but have some disadvantages, such as discomfort, instability, loss of taste, irritation of the mucous membrane, bone atrophy, etc.
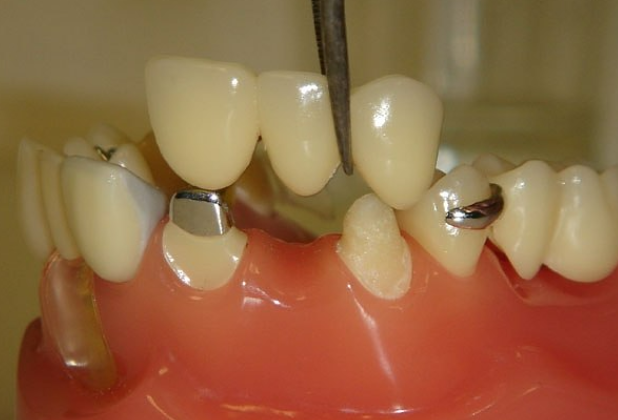
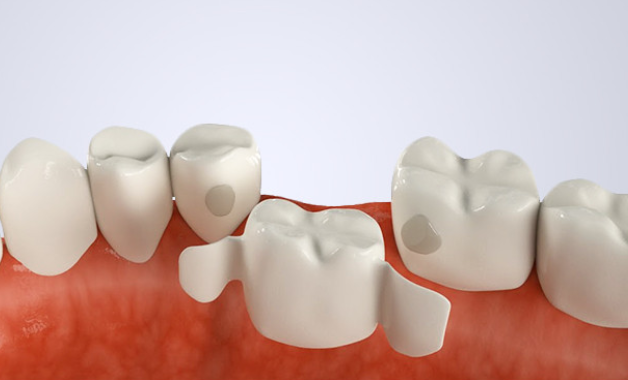
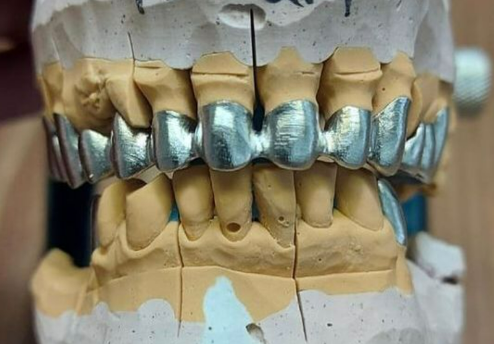
- Bridged prostheses. Bridges are fixed prostheses, which are fixed on the supporting teeth with metal or ceramic crowns. Bridges can restore the aesthetics and function of the teeth, but require grinding of the supporting teeth, which can lead to tooth damage, decay, pulpitis or periodontitis. In addition, bridges do not prevent bone atrophy at the site of missing teeth.
- Adhesive dentures are fixed prostheses that are fixed to the supporting teeth with a special adhesive that does not require grinding of the teeth. Adhesive dentures can restore the aesthetics and function of the teeth, but they have a limited lifespan, low strength and can cause mucosal irritation or hypersensitivity of the teeth.
- Minimally invasive dental implants. This is a new method of dental implantation that utilizes special smaller diameter implants that are inserted into the bone without a scalpel or sutures. Minimally invasive dental implants can shorten surgery time, reduce pain and risk of infection, and speed healing and rehabilitation. Minimally invasive dental implants can be a solution for patients with insufficient bone volume, but require a highly skilled surgeon and specialized equipment.
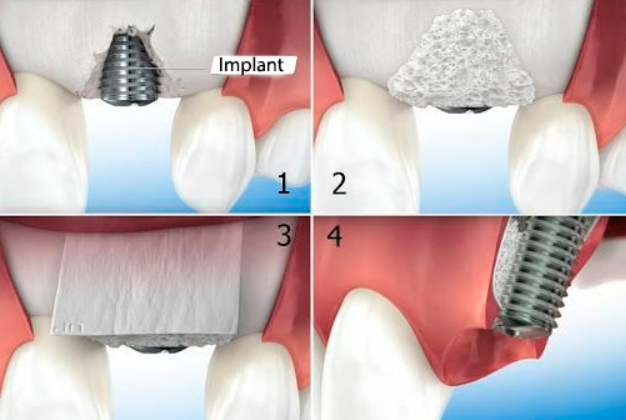
- Implantation of teeth simultaneously with directed bone regeneration. This is a method of dental implantation that uses bone material of animal origin and partially autogenous bone material, which stimulates the growth of own bone tissue at the implantation site. Dental implantation using bone substitute allows to increase the volume and density of bone tissue, as well as improve the osseointegration of implants. Dental implantation using bone substitute can be a solution for patients with bone atrophy, but requires additional time and cost, and may have some complications such as infection, inflammation, or rejection of the material.
Conclusion
Dental implantation is a complex and responsible procedure that requires an individualized approach to each patient. Patients with systemic diseases should be especially attentive to their health and consult with their primary care physicians before deciding on dental implants. In some cases, dental implants may be contraindicated or limited, but this does not mean that patients should give up their dream of having a beautiful and healthy smile. There are other options for restoring lost teeth that can be customized to the patient’s individual needs and capabilities. The main thing is not to be afraid to contact professional dentists who will help to choose the best treatment option and make the process comfortable and safe.